Millions of people live with migraine headaches-not just bad headaches, but debilitating events that can knock you out for hours or even days. If you’ve ever been trapped in a dark room, headphones on, trying to ride out the pounding pain while your body screams at you to move, you know this isn’t ordinary head pain. Migraines are a neurological condition, not a symptom. And while they vary wildly from person to person, the core problem is the same: your brain becomes hypersensitive, and small changes in your environment or routine can push you over the edge.
What Actually Happens During a Migraine?
It’s not just your head hurting. During a migraine, nerves in the blood vessels around your brain send pain signals. Your body responds by releasing inflammatory chemicals into the meninges-the protective layers around your brain and spinal cord. This inflammation is what causes the throbbing, pulsing pain most people associate with migraines. But it doesn’t stop there. Many people also experience nausea, vomiting, and extreme sensitivity to light, sound, and even smells. Some get warning signs minutes or hours before the pain hits-flashing lights, blind spots, tingling in the hands, or sudden food cravings. These are called auras, and they affect about 1 in 3 people with migraines.
One thing to remember: migraines aren’t caused by stress alone. Stress is a trigger, not the root cause. The real issue is that your brain’s pain system is on high alert. Think of it like a car alarm that goes off at the slightest touch. For some, a missed meal sets it off. For others, it’s a change in weather or sleeping in too long. The key is figuring out what sets off your alarm.
The Top Migraine Triggers (And How They Work)
There’s no universal list of migraine triggers because what sets one person off might do nothing for another. But some triggers show up again and again in studies and patient reports. Here are the most common ones-and why they matter.
- Stress: It’s the #1 trigger. Around 70% of people with migraines say stress brings on an attack. But here’s the twist: it’s not always during the stressful moment. Many people get what’s called a "let-down migraine"-the headache hits when the stress finally ends. Think: Monday morning after a busy weekend. Your body relaxes, your cortisol levels drop, and boom, the migraine starts.
- Sleep changes: Too little? Too much? Irregular hours? All of them can trigger migraines. Nearly half of all migraine attacks happen between 4 a.m. and 9 a.m., which suggests your body’s internal clock plays a big role. Skipping sleep on Friday, then sleeping until noon on Saturday? That’s a recipe for trouble.
- Hormonal shifts: For women, migraines often line up with menstrual cycles. About 65% of female migraine sufferers report attacks around their period. Estrogen drops right before menstruation, and that dip can be enough to trigger an attack. Pregnancy and menopause can also change your migraine pattern-sometimes making it worse, sometimes better.
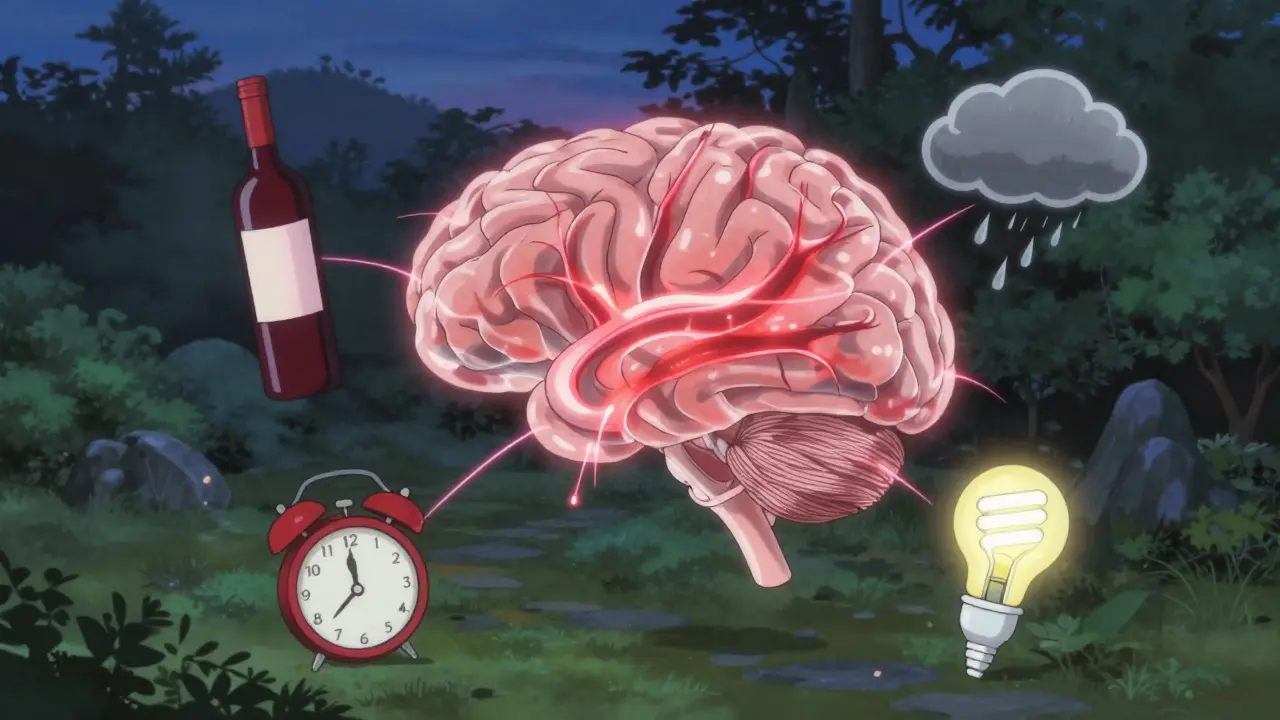
- Dietary factors: Foods aren’t always the culprit, but some common ones show up often. Alcohol (especially red wine), caffeine (both too much and withdrawal), MSG, aged cheeses, processed meats with nitrates, and artificial sweeteners like aspartame are frequent offenders. But here’s the catch: caffeine can also help. A small cup of coffee might stop an attack in its tracks for some people. That’s why keeping a food and symptom diary is critical-you need to know how your body reacts.
- Weather and altitude: Changes in barometric pressure, humidity, or even flying in a plane can trigger migraines. About half of sufferers report weather as a trigger. If you notice your headaches spike before a storm, you’re not imagining it. Low pressure systems affect blood flow and nerve sensitivity in the brain.
- Sensory overload: Bright lights (especially fluorescent or flickering), loud noises, and strong smells (perfume, smoke, cooking fumes) can all set off an attack. It’s not just annoyance-it’s a neurological overload. Your brain is already on edge, and these stimuli push it over the edge.
Here’s the thing: triggers rarely work alone. You might be fine with one stressor, but add poor sleep, a skipped lunch, and a bright office, and suddenly you’re in pain. This is called the "threshold theory." Your brain has a tolerance level. When enough triggers pile up, you cross the line. That’s why consistency matters more than perfection.
Preventive Medications: Stopping Migraines Before They Start
If you’re having migraines more than four times a month, or if they’re so bad they ruin your days, it’s time to think about prevention-not just pain relief. Preventive meds don’t cure migraines. They lower your brain’s sensitivity so triggers are less likely to set off an attack.
There are several classes of drugs used for prevention:
- Beta-blockers: Medications like propranolol and timolol were originally designed for high blood pressure. They work by calming overactive nerve signals in the brain. Many people see a 50% reduction in attack frequency.
- Anticonvulsants: Topiramate and valproate were made for seizures, but they also stabilize brain activity. Topiramate is one of the most studied migraine preventives and can reduce attacks by half in many patients.
- Tricyclic antidepressants: Amitriptyline is often used for chronic pain and sleep issues. Even if you’re not depressed, it can help by calming the nervous system and improving sleep quality.
- CGRP inhibitors: These are newer drugs-erenumab, fremanezumab, galcanezumab. They block a protein called CGRP, which plays a key role in migraine pain. These are injectable monthly or quarterly options with fewer side effects than older meds. They’re often used when other treatments fail.
Not everyone needs medication. For some, lifestyle changes alone are enough. But if you’re relying on painkillers every week, or if your migraines are getting worse, talk to your doctor about prevention. These drugs aren’t meant for occasional headaches-they’re for people who are stuck in a cycle.
Acute Care: What to Do When the Pain Hits
When a migraine is already in full swing, your goal is to stop it fast. The sooner you treat it, the better. Waiting too long makes it harder to control.
- NSAIDs: Over-the-counter options like ibuprofen or naproxen can work well for mild to moderate attacks. Take them at the first sign of pain-not after it’s already severe.
- Triptans: These are prescription meds like sumatriptan and rizatriptan. They work by narrowing blood vessels and blocking pain pathways. They’re highly effective for most people, but not safe if you have heart disease or uncontrolled high blood pressure.
- Gepants: Newer options like ubrogepant and rimegepant block CGRP during an attack. They’re great because they don’t cause rebound headaches like some older meds, and they’re safe for people with heart conditions.
- Anti-nausea meds: If vomiting is part of your migraine, your doctor might prescribe metoclopramide or prochlorperazine. These help with nausea and can also reduce pain.
- Caffeine: Yes, it’s a trigger-but it’s also a tool. Many migraine medications include caffeine because it boosts the effect of pain relievers. A small cup of coffee at the first sign of pain might help. But don’t overdo it-too much caffeine can backfire.
Don’t rely on opioids or codeine. They don’t work well for migraines, and they can make things worse over time by causing medication-overuse headaches. If you’re using painkillers more than 10 days a month, you’re at risk.
How to Track Your Triggers (And Why It Matters)
You can’t manage what you don’t measure. That’s why keeping a migraine diary is one of the most effective tools you have. You don’t need a fancy app. A notebook or even a notes app on your phone will do.
Each day, log:
- When you woke up and went to bed
- What you ate and drank
- Stress levels (on a scale of 1-10)
- Weather changes (if you notice them)
- Any sensory exposure (bright lights, loud music, perfume)
- Whether you had a migraine, and how bad it was
After a few weeks, patterns emerge. Maybe you always get a migraine on Tuesday nights after wine and late work. Or maybe your attacks spike every time the weather drops below 15°C. You can’t fix what you don’t see. And once you know your triggers, you can start avoiding them-or at least preparing for them.

What Doesn’t Work (And What You Should Avoid)
There’s a lot of misinformation out there. Here’s what you should skip:
- Detox diets: Cutting out entire food groups won’t cure migraines. Unless you’ve confirmed a specific trigger (like MSG or alcohol), you’re just making your life harder.
- Extreme sleep schedules: Sleeping 12 hours on weekends to "catch up"? That’s a trigger. Consistency beats quantity.
- Ignoring mental health: Anxiety and depression don’t cause migraines, but they make them worse. Therapy, mindfulness, or even just talking to someone can lower your overall sensitivity.
- Overusing painkillers: Taking ibuprofen or acetaminophen every day? You’re likely creating rebound headaches. These are headaches caused by the meds themselves.
There’s no magic bullet. But there is a path forward: know your triggers, stabilize your routine, and treat attacks early with the right tools.
Final Thoughts: It’s About Control, Not Cure
Migraines aren’t something you "get over." They’re a condition you learn to manage. The goal isn’t to eliminate every trigger-it’s to reduce the frequency and severity so they don’t control your life. For many, that means combining lifestyle habits with the right meds. For others, it’s just knowing when to rest, when to avoid the fluorescent lights, and when to take that pill before the pain fully sets in.
What works for your friend might not work for you. That’s okay. Your brain is unique. The more you understand your own patterns, the more power you have.
Can stress alone cause a migraine?
Stress doesn’t cause migraines on its own-it triggers them in people who already have a sensitive brain. But it’s the most common trigger, affecting up to 70% of people. Interestingly, many get migraines after the stress ends, not during it. This is called a "let-down migraine."
Are there foods I should avoid to prevent migraines?
Not everyone reacts the same way, but common food triggers include alcohol (especially red wine), aged cheeses, processed meats with nitrates, MSG, artificial sweeteners like aspartame, and caffeine (both too much and withdrawal). The key is tracking your own reactions-what triggers one person might do nothing for another.
Do I need to take preventive medication forever?
Not necessarily. Preventive meds are usually tried for 2-3 months to see if they help. If they reduce your attacks by half or more, you might continue. Some people can taper off after a year of stability. Others need them long-term. It depends on how often you get migraines and whether lifestyle changes alone are enough.
Can caffeine help or hurt with migraines?
Both. For some, a small amount of caffeine at the start of an attack can stop it. Many migraine meds include caffeine because it boosts pain relief. But regular caffeine use can lead to withdrawal headaches, and sudden cuts in intake can trigger migraines. Consistency is key-don’t skip your usual cup, and don’t overdo it.
What’s the difference between a tension headache and a migraine?
Tension headaches feel like a tight band around the head, are usually mild to moderate, and don’t come with nausea, light sensitivity, or aura. Migraines are more severe, often one-sided, and include neurological symptoms like vomiting, light sensitivity, or visual disturbances. Migraines can last hours to days; tension headaches usually resolve in a few hours.
Is there a cure for migraines?
There’s no cure yet, but there are effective ways to manage them. Many people reduce their attacks significantly by combining trigger tracking, lifestyle changes, preventive meds, and early acute treatment. The goal isn’t to eliminate every headache-it’s to regain control of your life.









RacRac Rachel
4 Mar, 2026
Just wanted to say THANK YOU for this post. I’ve been dealing with migraines for 12 years and this is the first time I’ve seen someone explain the "let-down" effect so clearly. I always thought I was just lazy after weekends… turns out my brain was just resetting. 🙌
Started tracking my sleep and stress levels last month and already noticed a 40% drop in attacks. Consistency > perfection, right? 💪
Jane Ryan Ryder
5 Mar, 2026
Wow another self help blog post about migraines. Next up: "how to stop crying when it rains". 😂
Callum Duffy
5 Mar, 2026
Thank you for the thorough and clinically accurate overview. I particularly appreciate the emphasis on the threshold model - it aligns with current neurology literature. Many patients are misled into believing single triggers are responsible, when in fact it is the cumulative burden that precipitates an attack.
For those considering CGRP inhibitors, I would advise discussing vascular history with a neurologist prior to initiation. Safety profiles are favorable, but not universally applicable.
Chris Beckman
7 Mar, 2026
i read this whole thing and honestly? caffeine is the real villain. stop drinking it. i used to get migraines every week until i quit coffee. now im fine. its that simple. why is this so hard to understand?
Levi Viloria
8 Mar, 2026
As someone who’s lived in three countries and experienced migraines in each, I can confirm: triggers shift with culture. In Japan, I noticed it was the fluorescent lighting in convenience stores. In Mexico, it was the sudden drop in humidity before storms. Here in the US? It’s the combination of stress, screen time, and overpriced kombucha.
There’s no universal answer - only personal patterns. This post nails it. Keep going.
Richard Elric5111
8 Mar, 2026
The metaphysical undercurrent of migraine - that of the body as an instrument of neurological dissonance - invites a deeper contemplation of agency in chronic illness. One might argue that the migraine is not an intrusion upon the self, but rather the self’s most authentic expression of systemic imbalance.
Thus, to treat a migraine with pharmaceuticals is not to heal, but to silence a signal. The true path lies not in suppression, but in attunement - to rhythm, to breath, to the quiet pulse beneath the storm.
Dean Jones
10 Mar, 2026
I’ve been reading up on this for years and I’ve got to say - most people don’t get it. Migraines aren’t about triggers. They’re about neural circuitry that’s been rewired by trauma, sleep deprivation, and modern life. You think it’s the wine? Nah. It’s the 18 months you spent working 80-hour weeks with no sunlight, then suddenly took a vacation.
People blame food, weather, hormones - but they’re just the match. The real fuel is the accumulated stress your nervous system has been storing like a battery. And when you finally relax? That’s when the battery discharges. That’s why let-down migraines are so common. Your body wasn’t waiting for stress - it was waiting for release.
And no, meditation won’t fix it unless you’ve also fixed your sleep schedule, your screen habits, and your emotional avoidance. You can’t out-mind a neurological condition. You have to out-structure it.
Track everything. Even the stupid stuff. Even if you think it doesn’t matter. Because your brain remembers what your conscious mind forgets.
And if you’re taking ibuprofen every day? You’re not managing migraines. You’re creating a new one. Medication-overuse headache is real. It’s called rebound, and it’s a trap. I’ve seen too many people stuck in it for years. Break the cycle. Talk to a specialist. Not your buddy who "got better after juicing."
Donna Zurick
11 Mar, 2026
I just started using the Migraine Buddy app and it’s changed my life. I thought I was fine until I saw my data - I was having attacks every 3 days and blaming everything but sleep. Now I know: if I go to bed after 1am, I’m doomed. Small changes, huge difference. You got this!
tatiana verdesoto
13 Mar, 2026
To everyone saying "just avoid triggers" - I get it. But what if you’re a parent? What if your job requires you to be in fluorescent lighting? What if your partner loves red wine and you don’t want to live separately?
This isn’t about perfection. It’s about awareness. I used to feel guilty every time I had a migraine. Now I say: "My brain is tired." And that’s okay.
You’re not broken. You’re not weak. You’re just wired differently. And that’s not a flaw - it’s a signal.
Thank you for writing this. It feels like someone finally saw me.
Jessica Chaloux
14 Mar, 2026
I cried reading this. 🥹 I thought I was crazy for getting migraines after a good night’s sleep. Turns out it’s the let-down. My therapist was right. I’m not broken. I’m just sensitive. And that’s okay. 💖
Mariah Carle
15 Mar, 2026
There’s a quiet poetry in the migraine - the way the world dims, the sound of your own breath becomes a drum, and the light, once a source of joy, becomes a blade.
It is not illness. It is revelation.
When your body screams, it is not asking you to fix it - it is asking you to listen.
Perhaps the greatest medicine is not in a pill, but in the stillness you refuse to ignore.
And if you’ve ever sat in the dark, trembling, and still chosen to breathe… you are already healing.